Table of Contents
Key Points
- Physical signs include changes in pupil size, bloodshot eyes, slurred or rapid speech, poor coordination, and unusual body odors, although these vary depending on the substance.
- Behavioral patterns, such as mood swings, secrecy, sleep changes, and missed responsibilities, become more revealing when observed consistently over time.
- One sign alone doesn't confirm drug use—look for clusters of symptoms and consider that many signs overlap with medical conditions.
- Emergency situations require calling 911, especially if you notice blue lips, slowed breathing, or an inability to wake someone.
- Approaching someone requires privacy, "I" statements about specific observations, and offering support rather than accusations.
- SAMHSA's National Helpline (1-800-662-4357) and the 988 Suicide & Crisis Lifeline provide confidential guidance for families seeking help.
It is essential to understand that you CAN’T tell, for certain, if someone is “high.” You may see physical signs which are consistent with drug use, or notice behaviors that are different from an individual’s characteristic behaviors, or suspect illicit use of drugs, but you can’t tell for certain without their admission of drug use or a drug test.
There are numerous physical and mental medical conditions that can be mistaken for the illicit use of drugs. Some of these include migraine headaches, stroke, and other neurological conditions. Depression, anxiety, psychosis, schizophrenia, and other mental health disorders may cause abnormal physical signs and uncharacteristic behaviors. Head trauma could be a problem. Metabolic disorders can show signs and symptoms characteristic of drug use. The most immediately threatening situations are associated with diabetes, such as very high blood sugar or diabetic coma, or an insulin reaction, often with dangerously low blood sugar. These situations call for emergency medical attention. Medication reactions can also mimic illicit use of drugs.
It is not useful to engage in heated arguments or accusations with someone showing signs and symptoms of illicit or inappropriate use of drugs, or a condition which can appear similar. These situations call for medical evaluation. If your suspicion for illicit drug use is great, remember that you can’t engage in rational dialogue with someone who is currently under the influence whose thinking is irrational. You also want to avoid triggering behaviors that may escalate to harm you or the person of concern.
Identifying drug use in people becomes more challenging when the person in question holds a special place in your life. Here, we’ll explain how to identify typical physical and behavioral indicators while showing you how to respond effectively and seek professional assistance when inappropriate drug use is suspected or diagnosed.
Read This First: Safety and Limitations
Many physical and behavioral indicators of drug use overlap with medical conditions, mental health symptoms, prescription medications, exhaustion, or normal adolescent development. A single sign doesn’t prove anything—what matters is observing clusters of symptoms over time [1].
Your role isn’t to diagnose. If you’re uncertain or concerned, seek guidance from a healthcare professional or contact SAMHSA’s National Helpline [2] at 1-800-662-HELP (4357).
EMERGENCY: When to Call 911
Call emergency services immediately if you notice:
- Blue or grayish lips, fingernails, or skin
- Slow, shallow, or absent breathing
- Choking sounds or gurgling
- Unable to wake the person
- Chest pain
- seizures
What to do: Call 911 first. If naloxone (Narcan) is available [3] and you suspect opioid overdose, administer it according to instructions. Turn the person on their side. Stay until help arrives—Good Samaritan laws protect those who seek emergency assistance from incurring legal consequences.
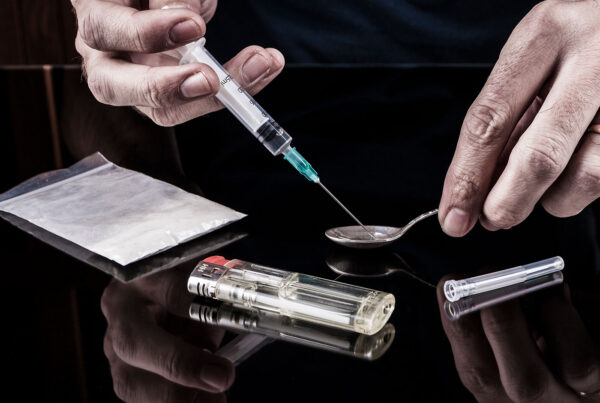
Physical Signs of Being High
Physical symptoms often provide the first clues. While these vary by substance, certain indicators appear [4] across different drug classes.
Common Physical Indicators
Eye Changes: Unusually large or extremely small pupils, red or bloodshot eyes, glassy appearance, and rapid eye movements.
Speech Patterns: Slurred words, excessively rapid talking, or disconnected speech.
Movement: Unsteady walking, poor balance, trembling hands, and difficulty with coordination.
Physical Symptoms: Excessive sweating, chills, nausea, dramatic appetite changes, and unusual odors (smoke, chemicals, solvents).
Signs by Drug Type: Quick Reference
Opioids (heroin, fentanyl, prescription painkillers):
- Extremely small (pinpoint) pupils, even in dim light
- Extreme drowsiness, “nodding off” repeatedly
- Slurred, very slow speech
- Noticeably slowed or shallow breathing
- May scratch skin frequently
Stimulants (cocaine, methamphetamine):
- Very dilated pupils, even in bright light
- Hyperactivity, inability to sit still
- Rapid, pressured speech
- Jaw clenching, teeth grinding
- Excessive sweating, rapid heartbeat
- May go long periods without sleep or food
Cannabis (marijuana, THC products):
- Noticeably red or bloodshot eyes
- Delayed responses, slower reaction times
- Increased appetite
- Distinctive smell on clothes or breath
- Some experience anxiety or panic
Depressants (benzodiazepines, sleep medications):
- Drowsiness, confusion, disorientation
- Markedly slurred, slow speech
- Severely impaired balance and coordination
- Memory problems
Inhalants (aerosols, solvents):
- Strong chemical smell on breath or clothes
- Irritation around nose and mouth
- Dizziness, unsteady movements
- Paint or chemical stains on hands or face
Behavioral and Environmental Clues
Behavioral patterns become significant when observed consistently over weeks or months, not as one-time occurrences.
Behavioral Patterns Over Time
- Unpredictable mood swings, increased irritability
- Lying about whereabouts, increased secrecy
- Dramatic sleep pattern changes
- Declining work or school performance
- Missing obligations, financial problems
- Suddenly spending time with new friends while abandoning old relationships
- Neglecting personal hygiene
- Withdrawing from family activities
Environmental Evidence
Drug Paraphernalia: Small baggies with residue, burnt foil, cut straws, syringes, glass pipes, unlabeled vape cartridges, and pill bottles without prescriptions.
Masking Evidence: Excessive air fresheners, incense, cologne, frequent eye drop use, constant mints or gum.
Note for Parents: Many signs overlap with normal teenage development [5]. Maintain open, non-judgmental communication and seek professional guidance if you are concerned.
What to Do: A Simple Decision Flow
Medical Emergency
If unresponsive, not breathing normally, or showing blue skin:
- Call 911 immediately
- Administer naloxone if available [3] for suspected opioid overdose
- Turn the person on their side
- Stay until help arrives
Concerning But Not Urgent
If impaired but conscious and breathing:
- Ensure safety—don’t allow driving
- Move to a calm, private space
- Stay calm, avoid confrontation
- Monitor for worsening symptoms
- Plan a supportive conversation when sober
- Research treatment options
Ongoing Pattern
- Document specific behaviors and dates
- Consult a healthcare provider
- Contact the Substance Abuse and Mental Health Services Administration’s (SAMHSA’s) Helpline: 1-800-662-4357
- Use family resources like “Talk. They Hear You,” a national prevention campaign from SAMHSA that offers resources like conversation starters, skill-building tools, and an app, designed to help parents and caregivers have early and effective conversations with young people about alcohol and other drugs
- Call 988 for crisis support
- Explore treatment programs
How to Talk with Someone You’re Worried About
Preparing:
- Wait until they’re sober and you have privacy
- Plan specific observations to discuss
- Gather treatment resource information
- Manage expectations—they may deny or refuse help
During Conversation:
- Use “I” statements: “I’ve noticed…” “I’m worried because…”
- Be specific: “I’ve noticed you’ve missed work three times this month.”
- Listen without judgment
- Offer support: “I’m here to help you get support.”
- Suggest an appointment with the individual’s healthcare provider to check for non-drug-related conditions
- Avoid enabling. Don’t make excuses or provide money
- Have realistic goals. Plant seeds, don’t force immediate change
Find Help
SAMHSA’s National Helpline: 1-800-662-HELP (4357) – Free, confidential, 24/7 support in English and Spanish
988 Suicide and Crisis Lifeline: Call or text 988 for emotional support and substance use concerns
FindTreatment.gov: SAMHSA’s treatment locator for facilities in your area
For Parents: SAMHSA’s “Talk. They Hear You” campaign and Partnership to End Addiction helpline: 1-855-378-4373
Finding Quality Treatment
Look for programs that are accredited, employ evidence-based approaches, offer individualized plans, involve families, have licensed staff, and provide aftercare support.
The Embers in Phoenix, Arizona, provides comprehensive outpatient treatment for substance use disorders and co-occurring mental health conditions, supporting both individuals and their families.
Moving Forward with Support
Recognizing signs of drug use is just the beginning. Substance use disorder is a medical condition requiring support, treatment, and compassion—not judgment. Your concern comes from caring, and that matters deeply.
If you’re worried about someone, trust your instincts. Reach out to professionals, use these resources, and don’t handle everything alone. You need education and support, too.
At The Embers, we understand how difficult these situations can be. Our outpatient programs in Phoenix provide comprehensive support for substance use disorders and mental health conditions, plus guidance for families.
Contact The Embers today to speak with our compassionate team about how we can support you and your family or a loved one on the path to recovery. You don’t have to face this alone.
Frequently Asked Questions
Sources
[1] Mayo Clinic. (2024). Teen drug abuse: Help your teen avoid drugs. https://www.mayoclinic.org/healthy-lifestyle/tween-and-teen-health/in-depth/teen-drug-abuse/art-20045921
[2] Substance Abuse and Mental Health Services Administration (SAMHSA). (2024). Helplines: Mental health, drug, and alcohol issues. https://www.samhsa.gov/find-help/helplines
[3] National Institute on Drug Abuse (NIDA). (2023). Naloxone DrugFacts. https://nida.nih.gov/publications/drugfacts/naloxone
[4] National Center for Biotechnology Information. (2024). Methamphetamine. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK535356/
[5] National Institute on Drug Abuse. (2025). Understanding drug use and addiction. NIDA. https://nida.nih.gov/publications/drugfacts/understanding-drug-use-addiction
Embers Recovery Editorial Guidelines
At Embers Recovery, we take your health and wellness seriously. We have a thorough process in place to ensure the integrity of information that is displayed on our website. All content published to our site undergoes a rigorous medical review by a doctorate level clinician to ensure medical accuracy.
Read More About Our Process